Authors: Christine Sekaggya-Wiltshire(1), Bruno Ledergerber(2), Amrei von Braun(1,2), Mohammed Lamorde(1), Allan Buzibye(1), Nadia Eberhard(1,2), Alexandra Scherrer (2), Rita Nakijoba(1), Daniel Muller(3), Lars Henning(2), Ursula Gutteck (3), Natascia Corti(4), Joseph Musaazi(1), Moses Kamya(5), Barbara Castelnuovo(1), Andrew Kambugu(1), Jan Fehr(2)
Affiliations:
- Infectious Diseases Institute, College of Health Sciences, Makerere University, Kampala, Uganda
- Division of Infectious Diseases and Hospital Epidemiology, University Hospital Zurich, University of Zurich, Zurich, Switzerland
- Department of Clinical Chemistry, University Hospital Zurich, University of Zurich, Zurich, Switzerland
- Department of Clinical Pharmacology and Toxicology, University Hospital of Zurich, University Zurich, Zurich, Switzerland
- Department of Medicine, College of Health Sciences, Makerere University, Kampala, Uganda
Background: HIV-positive patients co-infected with tuberculosis (TB) have anti-TB drug concentrations lower than reference ranges; however the relationship between concentrations of anti-TB drugs and treatment response remains controversial. We sought to evaluate if there is an association between low concentrations of first-line anti-TB drugs and delayed sputum conversion in a cohort of HIV-TB co-infected Ugandan adults.
Methods: We enrolled HIV-infected Ugandan adults diagnosed with first episode of pulmonary TB. Patients underwent pharmacokinetic sampling 1, 2, and 4 hours after drug intake to estimate the maximum drug concentrations (eCmax) at 2, 8, and 24 weeks of TB-treatment using high-performance liquid chromatography. Low concentrations were defined as an eCmax below the previously described cut-offs for rifampicin <8mg/L and isoniazid <3mg/L. Sputum conversion was defined as conversion of sputum culture or smear from positive to persistently negative results during follow-up. Cox regression and Kaplan- Meier curves were used to determine the association between sputum conversion dynamics and anti-TB drug concentrations.
Results: From April 2013 to May 2015, we included 226 HIV-infected patients with positive sputum cultures or smears at baseline. The median age was 34 years (interquartile range (IQR) 29;40), 58% (133) were male, the median CD4 cell count was 191cells/mm3 (IQR 70;333), and the median BMI was 19.1kg/m2 (IQR 17.6;21.6). The majority (177, 78%) of all patients was ART-naïve at time of TB diagnosis. Patients with low isoniazid and rifampicin concentrations were less likely to undergo sputum conversion before the end of follow-up compared to those with normal concentrations (HR:0.51; 95%CI:0.35-0.72; P<0.001 and HR:0.61; 95%CI:0.44-0.84; P=.003 respectively). In addition, patients with ≥ 1 drugs below the cut-off had a higher probability of remaining culture/smear positive over time compared to those with no drug below the cut-off (Figure). These associations remained unchanged in models adjusted for age, sex, and BMI.
Conclusion: Low isoniazid or rifampicin concentrations in HIV-TB co-infected patients resulted in delayed sputum conversion. This has potential implications on TB transmission.
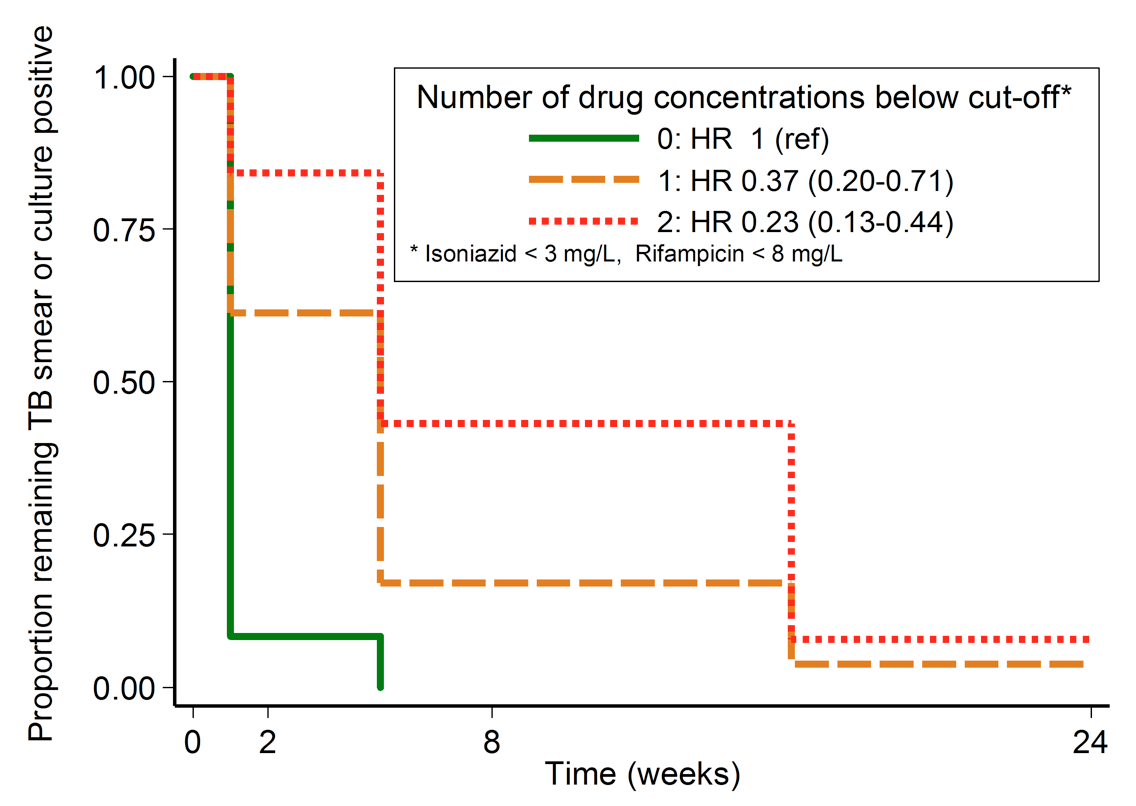
Figure: Kaplan Meier showing probability of remaining smear or culture positive over time among those with 0/1/2 drugs below the cut-off